Meet our heroes
These people are living with a rare disease and educating the wider public.
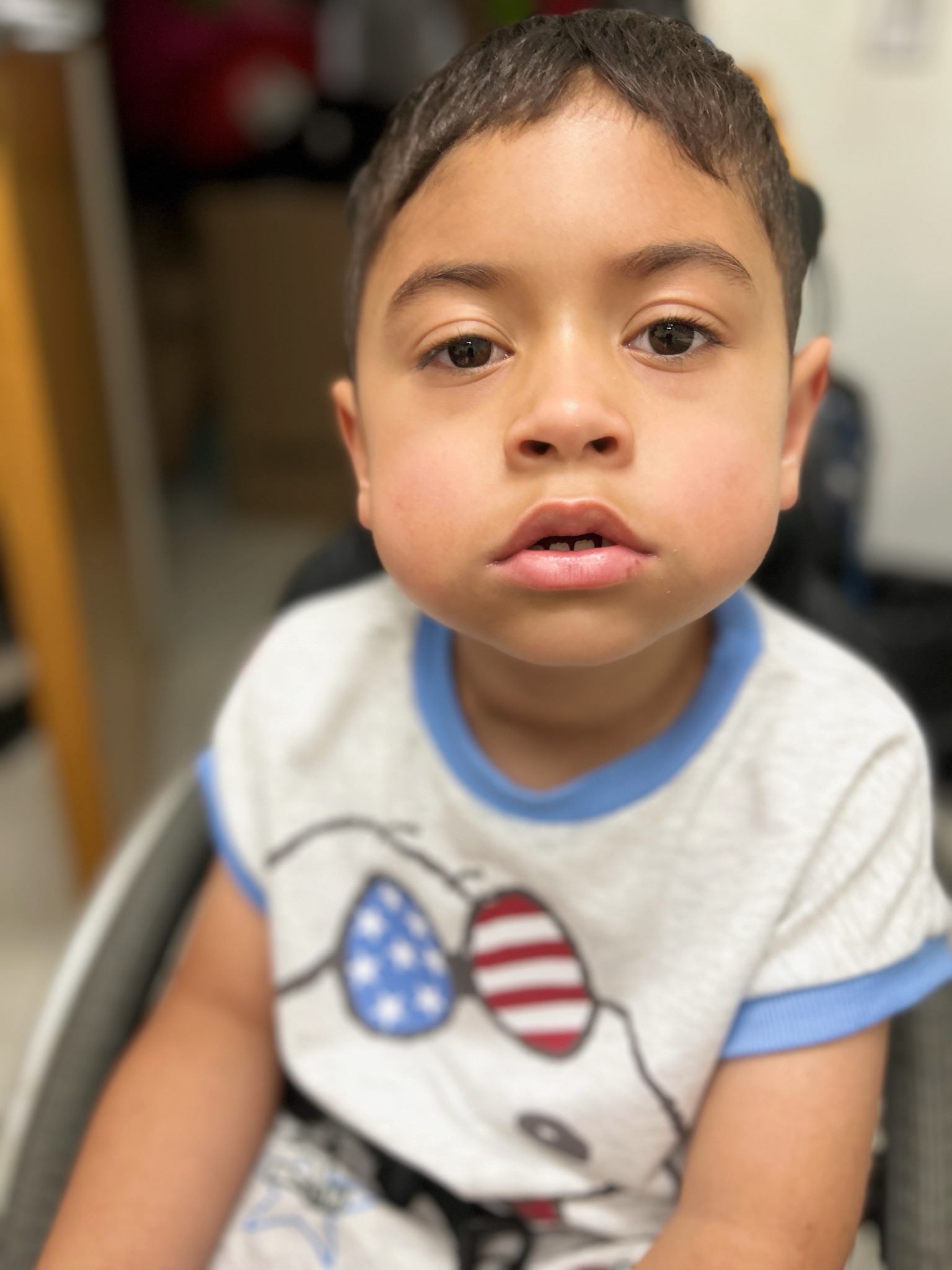
Vincent’s Story
In 2016 my son Vincent was born. Weeks after he was born he started experiencing symptoms of sweating, shaking, paleness and blueness in the lips… Continue reading Vincent’s Story
Read full story
Friends that Care are Rare
“Not Too Rare to Care” Did you know that millions of people are diagnosed with rare diseases and unknown disorders everyday, especially women? According to… Continue reading Friends that Care are Rare
Read full story
Living with Batten Disease: Anthony’s Story
Meet my son Anthony, he was diagnosed with Neuronal Ceroid Lipofuscinosis Type 7, also known as Batten Disease. Batten Disease is a rare, terminal genetic… Continue reading Living with Batten Disease: Anthony’s Story
Read full story
One in a Million
My name is Anna, I am 17 years old, and I am considered ‘one in a million.’ 10 years ago, I was diagnosed with Chronic… Continue reading One in a Million
Read full story
Reaprendendo a viver com Pompe
Sou Magda, 56 anos e tenho Doença de Pompe, uma doença rara, genética e hereditária que causa fraqueza muscular e dificuldade respiratória e apesar de… Continue reading Reaprendendo a viver com Pompe
Read full story
Facciolita and Primary Lymphedema
My Name is Nicole (or facciolita as my social media persona), and I was born with a rare genetic disorder called WILD syndrome that causes… Continue reading Facciolita and Primary Lymphedema
Read full story
Bringing awareness to #rarediseaseday, here is my son’s storytelling…
My name is Baptiste; I am 2 years old. I can already speak very well for my age, I am interested in many things including… Continue reading Bringing awareness to #rarediseaseday, here is my son’s storytelling…
Read full story
Famille sans sucre
Nous sommes une famille porteuse du gène CSID (DCSI). En effet j’ai 35 ans et en 2014 alors que je suis devenue maman pour la… Continue reading Famille sans sucre
Read full story
Léon
Notre fils Léon est atteint de la dystrophie musculaire congénitale type LAMA2, une maladie rare et orpheline d’origine génétique. Lorsqu’il a été diagnostiqué, les médecins… Continue reading Léon
Read full storyWhat's your story?
Be part of Rare Disease Day by sharing your story with others and sending a message of solidarity!
Share your story